Asthma
Asthma is a lung condition in which the airways are sensitive and react to triggers, causing breathlessness.
What is asthma?
What are the causes of asthma?
What are the signs and symptoms of asthma?
What are the possible tests and procedures for asthma?
What are the possible treatments for asthma?
What is asthma?
Asthma is a lung disease where the airways are more “twitchy” than usual. This causes episodes of breathlessness and wheezing when people are exposed to certain ‘triggers’ including allergens such as house dust mites, cigarette smoke or animals.
What are the causes of asthma?
While the exact causes of asthma are not well understood, asthma results from a tightening of airways (bronchial tubes) in the lungs.
Asthma causes changes to occur in the lungs:
- Airways become swollen, reducing airflow
- Contraction of the muscle layer within the airway, causing it to become tighter and narrower
- Mucus build-up inside the airways which can reduce airflow.
The image below illustrates asthma.
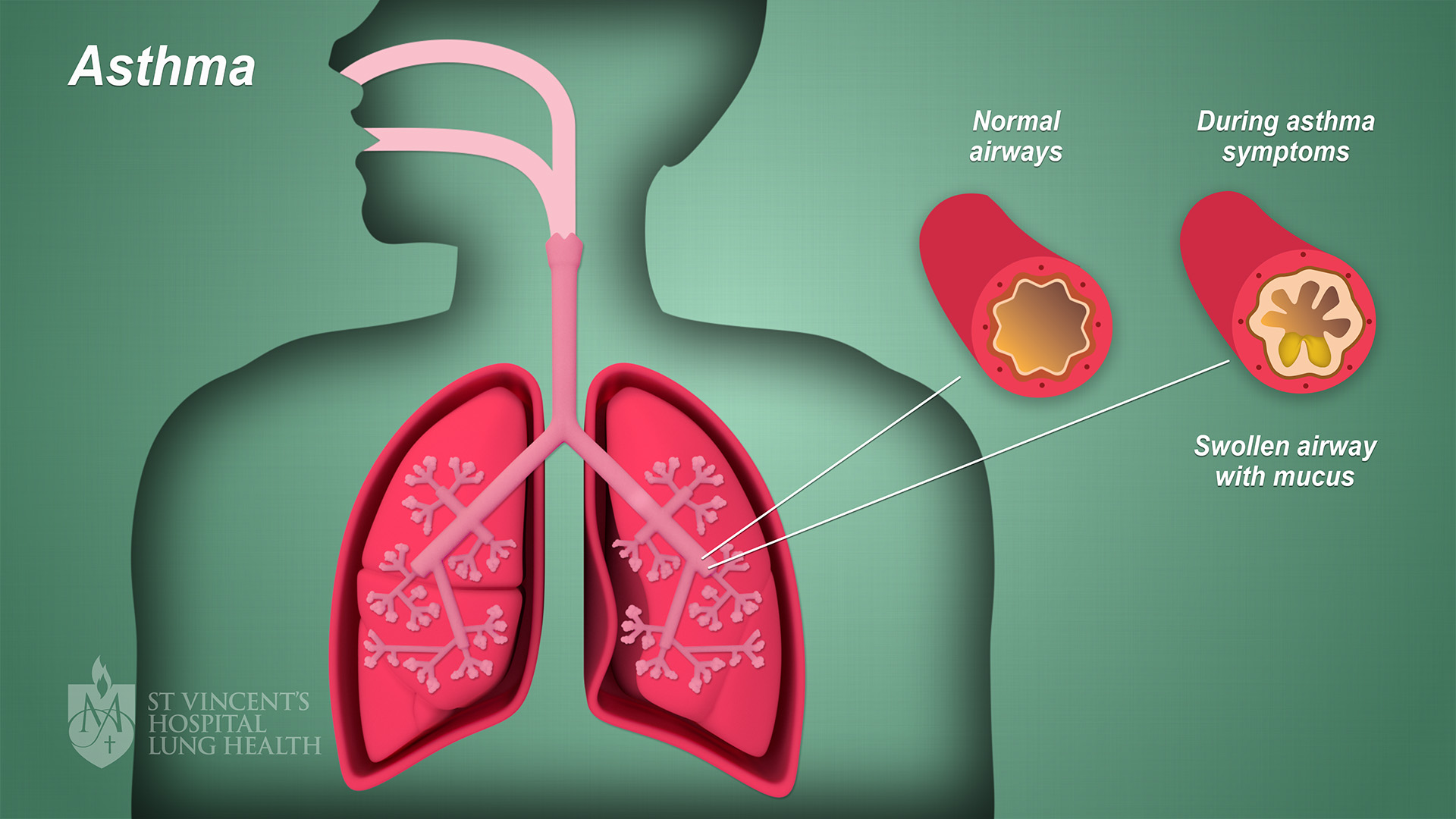
Common triggers for an asthma attack include:
- Allergies
- Cigarette smoke
- Colds and flu
- Extreme emotions, such as fear or anger.
What are the signs and symptoms of asthma?
Symptoms of asthma may be different for each person. Characteristically variable, symptoms can change daily and come on gradually over days or weeks. Symptoms that come on suddenly are known as an asthma attack.
Ideally, you should only have occasional signs of asthma. If your asthma is not well controlled, symptoms may be more frequent and you should see your doctor for a treatment plan.
Common symptoms of asthma include:
- Breathlessness
- Cough
- Early morning wakening with chest tightness
- Tightness in the chest, especially on exercise
- Wheezing.
Symptoms tend to be more common early in the morning and at night, or just after physical activity.
What are the possible tests and procedures for asthma?
While there is no one test to diagnose asthma, your doctor will ask about your medical history and asthma symptoms – how often they occur, and any possible triggers.
Some additional tests that your doctor may order are:
- Blood tests – a RAST (radioallergosorbent) test is a blood test that can measure your IgE (Immunoglobin E) which are antibodies produced by your immune system in response to potential allergens
- Chest X-ray – used to rule out other potential conditions that cause asthma-like symptoms (such as pneumothorax) or to identify rare types of asthma (such as allergic bronchopulmonary aspergillosis)
- Fractional exhaled nitric oxide (FeNO) – this breath tests assess the inflammation in your airways and can assist with monitoring your treatment
- Peak expiratory flow rate (PEFR) – monitors your lung function; if you have asthma, lung function will typically vary over time
- Skin prick tests – involves making small pricks to the skin of the arm, and presenting common allergens (such as dust mites, grass pollens, moulds and some household pets) in small quantities; reactions from the skin prick test can identify potential allergies that trigger asthma
- Spirometry – a lung function test that measures the amount of air breathed in (inhalation) and out (exhalation) before and after taking a type of asthma medication (known as bronchodilator, which makes your airways larger); if lung function improves after medication, it is likely that a diagnosis of asthma will be made (spirometry can also be used before and after exercise to diagnose asthma that is induced by exercise).
What are the possible treatments for asthma?
Treatment and management of asthma typically involves a combination of medication, education and lifestyle changes. Work with your doctor to find an asthma management plan that works for you, so you can:
- Avoid flare-ups and night time awakenings due to asthma
- Lead a lifestyle that is as healthy as possible
- Tolerate asthma medication without severe side-effects
- Tolerate exercise.
Asthma Management Plan
The treatment of asthma in Australia has been developed by the National Asthma Council, and it is aligned around the 6 Step Asthma Management Plan:
- Assess the severity of the asthma – this can be done via the use of spirometry or other lung function measures, as well as assessing your symptoms and how they impact on your daily life, your medication needs as well as any admissions to hospital
- Achieve best lung function – this can be achieved by minimising asthma symptoms, usually by the use of medications (it may take some time to find the dosage that is right for you and your asthma)
- Identify and avoid trigger factors – so that you can avoid potential allergens (such as dust or cigarette smoke) that could trigger asthma flare-ups
- Maintain best lung function with optimal medication – this will typically involve medications that reduce any potential side effects such as ‘relievers’ and ‘preventer’ medications, as well as regular monitoring of lung function and asthma symptoms
- Know your action plan – this is a plan formulated with your doctor, so that you can be prepared for situations when you have asthma flare-ups, and know when to seek medical attention, if necessary
- Check your asthma regularly – regular monitoring of your asthma is important, even if your symptoms are under control, this is to ensure current medications and treatment plan is still appropriate.
Medications for asthma
Relievers
Relievers can be inhaled either from a puffer (with or without a spacer) or from a nebuliser, where medication is administered via a spray mist and breathed in. Relievers are bronchodilators (they make the airways bigger) and they work by relaxing the muscles around the airways in the lungs. Relievers are taken when an asthma attack occurs, as well as before exercise for people who have exercise-induced asthma.
Preventers
Preventers aim to reduce and prevent inflammation of the airways. Corticosteroids are common and effective preventer medications. Preventers are taken via a puffer and should be taken on a regular basis, regardless of asthma symptoms. There are also some tablets available as preventers, and desensitisation to allergens, but these may not be paid for by the PBS.
Symptom controllers
Symptom controllers deliver long-acting reliever medications via a puffer once or twice a day, depending on symptoms. They are designed for people who suffer from more severe asthma.
If you are prescribed a puffer, it's important to use it correctly so that your lungs can benefit from the medication. Read through the National Asthma Council of Australia's Inhaler Checklist to see if you are using your puffer correctly.